By Meleni Aldridge BSc Nut Med, AFMCP™ Graduate
Executive coordinator
"We have entered an era of 'metabolic terrorism' — what we are doing to ourselves is literally metabolic terrorism." Mark Hyman MD, chairman Institute for Functional Medicine.
It's a melancholy thought that the majority of people today are eating themselves into chronic disease. It's just that they don't know it or perhaps don't want to know it. Ignorance may be bliss sometimes, but not when you're playing Russian roulette with your health. By the time we reach our 40's, 60% of us in the developed world will have some degree of CardioMetabolic Syndrome (CMetS). In plain English, the syndrome encapsulates the obesity, diabetes and cardiovascular disease (CVD) epidemic that accounts for a monumental, but largely preventable, death rate. Mark Hyman indicated that the US is forecast to spend US$47 trillion over the next 20 years dealing with chronic disease – which is primarily a 'food-borne' illness. We have eaten ourselves into this position and now we need to eat ourselves out of it. Food is not a substitute for medicine, it simply is the best medicine.

850 delegates attend IFM's annual conference: The New Era – Cardiovascular Disease, Metabolic Syndrome and Obesity - Scottsdale, Arizona 31st May - 4th June 2012
IFM's most successful conference
The Institute for Functional Medicine (IFM) convened its annual conference in Scottsdale, Arizona last week. The largest conference in IFM's history saw 850 practitioners, many of them doctors and cardiologists, come together to explore 'The New Era – Cardiovascular Disease, Metabolic Syndrome and Obesity'. Heart disease remains the No. 1 killer in the US and many other countries. Despite the wealth of evidence and extensive resources devoted to the management and treatment of CVD, it is still the most prevalent disorder. Given the multifactorial nature of the disease, the new term CardioMetabolic Syndrome (CMetS) has emerged to describe the complex interconnectedness of the elements involved. Elements that demand a new approach rather than a simplistic 'pill for an ill' drug-based approach. Enter the new functional medicine systems biology paradigm.
Healing the heart
Dr Mark Houston, aptly described as a 'tour de force' by IFM co-founder, Jeffrey Bland PhD, and a biological and physiological genius by Kristi Hughes ND, was one of the main speakers at the conference. Throughout the 4-day conference, delegates were treated to 10 hours (and an eye-watering 1161 presentation slides!) detailing Dr Houston's unique and profound knowledge of CMetS. However, as transfixing as the information was, the experience was a little like drinking from a fire hose!
Amongst the exquisite clinical pearls revealed over the 4 days, we were reminded that the heart is so much more than just a pump for our blood supply. Along with the arteries and blood vessels, our cardiovascular system represents the largest organ in our body. Its vital functions are maintained by a massive array of interconnected neurological (nervous), endocrine (hormonal) and immune system functions and feedbacks. It is intimately involved with general metabolic function, so what you eat, how you eat, how you move and exercise, how you feel emotionally and, generally, how you live your life, impacts and affects your heart profoundly. What has been known for eons in traditional systems of healing is that healing the heart means treating the whole person. You cannot separate the emotional, spiritual and psychological aspects of someone from the physical aspects, which is why you can never heal cardiovascular disease with a purely drug-based approach. Human beings are social animals. We are designed to live in partnership within supportive communities. With the increasing disintegration of the fabric of modern society and the ensuing isolation experienced by many, is it any wonder that heart disease has become the No. 1 killer in the Western world?
Paradoxically, heart disease is a complete unknown for indigenous hunter-gatherer populations still living in communities, eating their traditional diet and maintaining the activity levels of their origins. As cardiologist Mimi Guarneri reminded us during the conference, it's all about connection, coherence and harmony and to never forget the important contribution that social connection makes to our health. Getting centred, focused and relaxed, and making space to create relationships, are all important pieces in healing the 'broken heart' of today’s society.
Back to basics: important fat stats
Not all fat is created equal. Depending on where your fat is deposited, it can be 'angry' or 'friendly'. And there is also such a thing as 'skinny fat' — you don't need to be overweight to have angry fat and be at risk of CMetS! Would it surprise you to find out that you're more likely to be overweight if your friends are overweight than if your parents are overweight? Epigenetics – the way we respond to our environment – always wins out over genetic inheritance, which should be good news as it also means you can change your health and read a different page in your genetic ‘book of life’. This is yet another reason why chronic disease should be considered a social disease, with the impact of social networks on health taken into consideration. So why is there so much fuss made about being overweight and why such focus on fat?
Eating a diet loaded with inflammatory foods (e.g. high trans fats, high sugar, simple refined carbohydrates, processed and junk foods) combined with a lack of adequate physical activity, will raise your blood sugar levels, imbalance your insulin levels (your fat storage hormone) and cause more body fat to be laid down. Adding stress into the mix raises your stress hormones as part of the ancient fight and flight mechanism, which is all very well if the stress is short-lived, but creates further problems if chronic. Most modern stress is chronic, meaning regularly repeated and long-term, causing metabolic dysfunction in our sugar and fat regulation. That's why many people gain weight when they are long-term stressed and particularly gain it around the middle.

Mark Houston MD delivering his last lecture to the 850 delegates at IFM's annual conference, Scottsdale, Arizona
Belly fat caution
The belly fat that causes your waistline to increase is most typically the 'angry' fat, which pumps out inflammatory signals and initiates a full immune system reaction that in turn finds it harder and harder to differentiate between friend or foe. The immune system doesn't differentiate between being chased by a sabre-toothed tiger, your belly fat or your bank manager! The result is the same, the generation of oxidative stress (free radical damage), autoimmune vascular dysfunction (damage to blood vessels), endotoxaemia (internal toxicity) and inflammation.
Belly fat contains both subcutaneous (under the skin) fat and fat inside the abdominal cavity. It's the fat in the abdominal cavity that is termed visceral adipose tissue (VAT). It's the most dangerous type of fat you can have because not only does it function in a hormonal way, triggering the immune system, but it also spills over and starts infiltrating the organs. Organs disabled by fat can't work properly and we are seeing an exponential rise in non-alcoholic fatty liver disease (NAFELD). This is basically cirrhosis of the liver from eating the wrong diet, rather than consuming too much alcohol. The fact that we are now seeing children with NAFELD, type II diabetes, CVD and strokes is just wrong, wrong, wrong. And completely preventable – it just shouldn't be happening.
As Dr Shilpa Saxena put it, "feeding kids in such a way that they're getting overweight at an early age is just cooking the diabetic fire for them in later life".
A food-first approach – the power of the fork
Putting the fire of inflammation out is critical in addressing CMetS and halting the progression from overweight to obesity, to diabetes and/or CVD. The good news is that food is your best medicine — even type II diabetes can be successfully treated in 12 weeks with the right nutrition and exercise protocol.
Just as all fat is not created equal, neither are calories. Consuming 1000 calories of soda or junk food has a totally different effect on the body than consuming 1000 calories of broccoli. Everything you eat needs to be regulated by your biology and has an influence on your cells and your genes. Eating a healthy diet with a low glycaemic load (GL) means you burn around 300 calories more than eating the same calorie load of high GL foods such as sodas and junk food. Quite simply, the healthier your diet, the more you burn calories before you've even started lacing your trainers!
Risk factors
The three central components underpinning CMetS are oxidative stress, inflammation and autoimmune dysfunction. All are modifiable with diet and lifestyle changes. CMetS is a complex disease pattern for which Mark Houston MD has identified around 400 individual risk factors involving a multitude of biochemical and physiological pathways in the body. Trying to block one or more of these pathways, the typical objective of drug development, leads to a very high likelihood of side effects because the pathways are interconnected and interactive. But since the these pathways have co-evolved with food, as nature intended it, putting in the right combination of nutrients in the diet can have restorative effects on health in ways that can’t be matched by drugs. Food is truly the best medicine.
Although with the stranglehold the drug companies have on conventional medical education, millions of patients are still routinely getting prescriptions for statins, blood pressure meds and diabetic drugs from the off rather than being given the nutritional and lifestyle protocols they so badly need. Being cynical, the lack of interest shown by mainstream medicine is down to the fact that nutritional and lifestyle factors can't be patented!
Risk factors differ for men and women. Women are at risk from higher triglyceride levels and inflammation, as well as having differing risk pre-menopause and post menopause. Once a woman has gained a certain amount of belly fat and becomes more ‘apple-shaped’ than ‘pear-shaped’, there is a hormonal shift too to a more male pattern with higher testosterone levels than are normal. It's this 'male pattern' that causes women to have high blood pressure and CVD. Men on the other hand suffer testosterone deficiency syndrome, which is a result of VAT, chronic stress, high insulin levels and a hormonal shift to a more 'female pattern' with higher oestrogen levels. Men who are converting their testosterone to oestrogen because of metabolic dysfunction end up developing 'moobs' (‘man boobs’) and suffering mood swings, amongst other metabolic disturbances. Both sexes literally turn topsy-turvy.
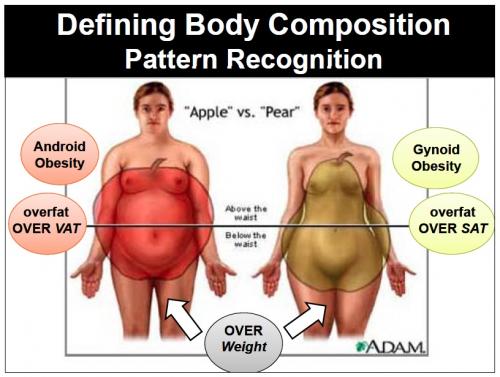
Source: Shilpa Saxena MD, IFM Faculty
Closing thoughts
This wasn't just another medical conference, this is a movement and it's heralding a new paradigm in healthcare. A new era and a new vision of how we manage our health. There are many of us that know this, see it and are part of it – it's just taking a bit of time for conventional medicine and the industry that supports it to welcome in the inevitable!
One of Dr Mark Houston's take home points during the conference was that the appropriate lifestyle, non-pharmacologic, pharmacologic (in acute care) and integrative therapy, need to be delivered earlier — before the onset of clinical disease. It was so refreshing to see a doctor of his stature with slide after slide of food-based, non-drug treatment regimens. Although he did also mention that his approach has meant that he's in a lot less demand for speaking at some conferences!
In closing it seems pertinent to share the final words from Kristi Hughes ND, the incredible woman, wife, mother and clinician responsible for organising this outstanding IFM conference:
"I can do this,
You can do this,
Together we can all change the world."
10 steps away from CardioMetabolic Syndrome
- Keep your blood sugar balanced through eating sufficient good quality protein, unprocessed whole foods rich in vegetables and some fruits – eat a rainbow every day. Limit starchy carbohydrates and consider a 'grain holiday' for your body
- Don't drink your calories in sodas, fruit juices or excessive alcohol. Ensure that you're adequately hydrated with pure, clean water every day. Constantly drinking throughout the day upsets our homeostatic balance related to thirst, so try to bulk water drink when you get thirsty instead. Aim to consume a minimum of 1.5 L per day, but more if you're very physically active or live in a hot climate
- Have 2-3 protein and fibre-rich meals per day, with at least a 5 hour fast between meals – avoid snacking!
- Find out if you have any hidden food allergies that may trigger cravings. Dairy, wheat, gluten, eggs and nuts are some of the main allergen foods. If you feel that any of these (or other foods) may be a trigger for you, try eliminating it for 4 weeks and then reintroduce to see if you have any specific reaction
- Get moving – there is no substitute for daily activity! You need at least 40 minutes to an hour a day of moderate to intense activity and outdoors is best if you can manage it. Always remember that the resistance (weight-bearing) work should come first before the aerobic exercise.
- Get 7-8 hours sleep every night and make an effort to get to bed by 10 pm
- Optimise your nutrient levels – always food first and then supplement if necessary. Ensure you're getting enough vitamin D and Omega 3 fats from oily fish (or from plant or microbial sources if vegetarian, although this is much harder to achieve)
- Implement some stress transformation strategies – meditate before you medicate! Find what works for you, anything from breathing techniques to yoga, to zumba classes, to hill walking, to mountain biking can be meditative and relaxing if it lets you forget time and get ‘out of your head’
- Prioritise your personal purpose and meaning in life and do what you can to pursue it. Remember you are a multidimensional individual with a complex of mental, psychological, emotional, spiritual and physical needs. They are all equally important.
- Lastly, seek professional support and treatment if you are concerned about your health or your heart. Find a functional medicine practitioner who has completed the Institute for Functional Medicine's 5-day course, Applying Functional Medicine in Clinical Practice. Whilst this is predominantly a US list of practitioners, there are also some practitioners listed from other countries, UK included.








Comments
your voice counts
There are currently no comments on this post.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences