By Robert Verkerk BSc, MSc, DIC, PhD, FACN
Founder, executive & scientific director, ANH-Intl
As I returned from Sierra Leone on Sunday night, I was reminded how effectively fear has been generated in the population at large.
After disembarking from my Royal Air Maroc flight with Sierra Leonan colleague Morris Marah, I got to the immigration counter at London Heathrow Terminal 4 and gave my passport to my allocated immigration officer. With my passport was the folded declaration document duly completed, as required by all travellers returning from any of the Ebola-affected West African nations. When the immigration officer opened the document and saw what it was, he forcefully pushed his chair back to distance himself from me and exclaimed, instinctively, “Get back, stand back, you’ve got Ebola.” I responded calmly, saying, “Indeed I don’t believe I have, and you’ll be aware that if I did, I couldn’t possibly give it to you as I am expressing no symptoms. And if I was, we would have to have body contact and exchange body fluids.”

The immigration officer pulled himself together as quickly and professionally as he could, and somewhat embarrassingly agreed that was probably the case. He then pointed me in the direction of the health screen for Ebola. The operation at Heathrow and Gatwick airports as well as Eurostar terminals are set to cost UK tax payers £9 million over the next six months. Following my health screen and a lengthy discussion of my proximity with Ebola patients in Sierra Leone, the medics agreed to let me go on the condition I record my temperature daily and self-report back to Public Health England should my temperature rise above 38.5oC. This, in my opinion, is altogether a more rational approach than the enforced quarantine used in the USA.

Ebola poster. Teaching people how to avoid infection is key to breaking the transmission cycle. So far, it’s the most proven form of ‘medicine’
We’ve been staying partially under the radar for the last few weeks while we’ve been studying diverse aspects of the Ebola crisis, taking soundings from various places and building alliances in West Africa. But there are a few things that we can no longer stay mute on, and we feel compelled to communicate these issues widely. Mainstream media isn’t telling the truth about what’s really going on on the ground. Not for the first time, we’re choosing to use our website, social media and the millions we communicate to in this way, including increasing numbers in West Africa, to get some key information across about Ebola that you won’t probably have heard from mainstream media.
We believe there are six main points that have been either not widely communicated or have been miscommunicated. These are:
1. Contracting Ebola does not mean probable, or even 70% likelihood, of death, in contrast to what the WHO has been telling us. In fact, in Sierra Leone, official WHO and CDC figures show that infected individuals only have between a 20% to 25% chance of death. These may be under estimates based on under-reporting of deaths, but given the amount of monitoring going on, it would seem highly unlikely that every in one in two deaths are unaccounted. Few will have missed the many citations claiming 70% mortality following infection by Ebola. The WHO assistant director-general Dr Bruce Aylward said in a news conference last month that the mortality was 70% and was almost identical in the three hardest hit countries Liberia, Guinea and Sierra Leone. If you look at the most recent WHO figures (up to 17 November 2014) you’ll find the mortalities from all known cases (confirmed, suspected and probable) are 59%, 42% and 20% for Guinea, Liberia and Sierra Leone, respectively (Table 1). The figures are not that different if you look only at confirmed cases (Table 1).
Table 1: Confirmed, probable, and suspected cases in Guinea, Liberia, and Sierra Leone
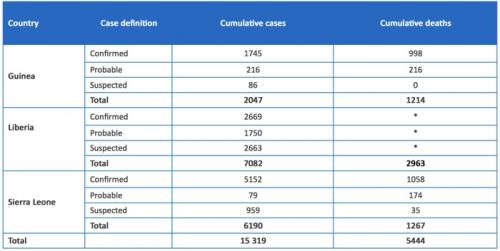
Data are based on official information reported by the Ministries of Health of Guinea and Sierra Leone up to the end of 18 November, and the Ministry of Health of Liberia up to the end of 17 November. These numbers are subject to change due to ongoing reclassification, retrospective investigation and availibility of laboratory results. *Data not available.
Source: http://www.who.int/csr/disease/ebola/situation-reports/en/
2. There are huge disparities in death rates between the three key West African countries that have been at the centre of the Ebola outbreak. The figures above (Table 1) show this, with Sierra Leone showing an apparently better survival rate than any of the other three countries. Again, not much has been said about this publicly. There could be many reasons for this tendency, including the fact that Sierra Leone reporting is less accurate, or that, as the last of the three countries to suffer major outbreak, Sierra Leone may be benefiting from reduced vigour in the viral strain. There may also differences in the (human) host (immune) response. That, in turn, can be linked to health, nutritional and hydration status of infected individuals. Quite possibly it’s a combination of several or many things, but it certainly suggests that there are opportunities to enhance the immune response and improve survival rates. Strengthening the host has not been in the vocabulary of the international agencies dealing with the epidemic. Most of the effort has so far either gone into breaking the transmission cycle or killing or inoculating against the pathogen.
3. Based on current figures, a person is about 200 to 1200 times more likely to die of malaria than Ebola. If you compare cumulative risk of death from malaria, based on figures published in The Lancet, with those from Ebola, you’ll get the following results (Table 2). Interestingly, the risk of death from Ebola is considerably higher (4- to 8-fold) than in Guinea or Sierra Leone. But once again, malaria, as the most serious infectious disease in Africa, gets pushed to the backwaters of healthcare. Mainly, it would appear, because there is no hopeful drug to treat it on the horizon. Ebola, on the other hand, has a clutch of vaccines, antivirals and blood products. in the pipeline.
Table 2. Cumulative risk of death (per thousand population) from malaria and risk of death from Ebola (as of 17 November 2014)
| Risk of death | Guinea | Liberia | Sierra Leone |
|---|---|---|---|
| From Ebola | 0.1/1000 | 0.85/1000 | 0.2/1000 |
| From malaria | 122/1000 | 158/1000 | 152/1000 |
| Increased likelihood of death from malaria compared with Ebola | 1110-fold | 186-fold | 690-fold |
Malaria figures derived from The Lancet, Ebola figures from the WHO, and population data from the World Bank.
4. Millions being donated to support the Ebola relief effort are not getting to local community holding centres in Sierra Leone, the country which is currently carrying the burden of the West African outbreak. My colleague, Morris Marah, a Sierra Leone crisis management expert, and myself, have just returned from an 8-day mission to Sierra Leone. We were, and continue to, work closely with Sierra Leone government authorities. We were shocked by the fact that not even a trickle of funding had arrived to fund the community holding centres, 200 of which are being built around the country. Find out more in our press release issued yesterday.
5. WHO guidelines are killing people. The WHO guidelines that currently apply to Ebola treatment and holding centres propose avoiding intravenous support for Ebola patients, despite the fact that dehydration from the potentially lethal fluid loss associated with the disease is one of the disease’s hallmarks. The Sierra Leonean medical team at the Hastings treatment centre just outside Freetown has found that survival rates can be increased by 20% simply by introducing intravenous fluid replacement, broad spectrum antibiotics and multivitamins. Find out more.
6. Waiting for vaccines, antivirals or other drugs is not the only intervention that will save lives. The WHO upholds that no effective treatments are currently available for Ebola.Tulip Mazumdar, global health correspondent for the BBC in Conakry, Sierra Leone, pronounced yesterday, “At the moment, medics can only treat the symptoms of Ebola, giving people pain relief and keeping patients hydrated in the hope they will be strong enough to fight the virus off themselves.”
The WHO tells us there are two vaccines, two antiviral drugs and two blood products in the pipeline, and we assume we are meant to be welcoming their arrival with open arms.
Based on the latest knowledge of what is happening in Sierra Leone, there is a good chance that intravenous therapy coupled with oral nutritional protocols could transform outcomes. Dr Sesay’s experience at the Hastings treatment centre has already improved outcomes by 20%. How many more lives could be saved by protocols that are already available and common place in the field of integrative and functional medicine?
Under the banner of the International Sanitation Response on Ebola (ISRE), with the guidance of a team of leading integrative medicine clinicians, notably from the USA, we have committed to support Sierra Leonean health authorities in their bid to improve outcomes for their own people. Critical to this is to increase resources available to construct adequate holding and treatment facilities and to improve the quality of care, given the lack of any current support from aid agency funding or donations from Western ‘Ebola relief’ campaigns.

A lady survivor in the village of Kigbal who lost her 4 children and husband to Ebola, and still has two remaining children fighting for their survival in a treatment center
Urgent funding appeal
With so much money pouring into the current efforts, no diversion of funds towards efforts that improve immune system response to the virus are likely to occur. We are thus forced to urgently raise funds to start trials independently and have an initial funding target of US$250,000. We will be working alongside Sierra Leonean medics in Ebola holding and community centres built to receive Ebola patients. Funds are required to purchase and freight equipment, lab tests, protective equipment, communications, transport and logistics. Should individuals, organisations or companies wish to donate, please contact us, quoting your interest in ‘ISRE’.
NB: Please type ‘ISRE’ in the ‘Note to Seller’ field, which will show on the Paypal payment page whether you are using your own Paypal account or paying by credit card.
For other donations, please contact:
Sophie Middleton, campaign administrator, email [email protected] or tel +44 (0)1306 646 600.

Inside the Hastings treatment centre, outside Freetown, Sierra Leone
Ebolagate
The six points of misinformation or miscommunication that we’ve raised in this piece justify, in my view, use of the title ‘Ebolagate’. We could have raised many more points, but we’re highlighting these for impact. We’re not the first to use the term; the journalist Jon Rapporport and others have used it before us, but have raised different issues.
There is no doubt in my mind that Ebola—for all the pain and suffering it causes affected communities—has sadly become both a political and psychological tool manipulated by third parties. It seems that the aim among those controlling the international ‘relief effort’ is about maintaining the dependence of West African nations on Western nations and solutions. It’s an extension, I believe, of the control that has been exercised by Western governments, aid agencies or transnational corporations, both after the ‘scramble for Africa’ and since many African countries reclaimed their independence in the 1960s.
It needn’t be this way, but by us falling victim to the manipulation, we become part of the problem, not the solution.
We must each make up our own minds, and figure out if we can, or should, help. And if so, we must decide what form that help might take. I for one, believe the ISRE project could make a big difference. That’s why I’m so committed to the project.








Comments
your voice counts
26 November 2014 at 8:02 pm
Dr Sircus has done some extremely helpful research into integrative approaches to Ebola treatment, including the use of selenium, magnesium, high potency Vit C, Vit D, iodine, infrared therapy and glutathione. Information well worth disseminating.
http://drsircus.com/medicine/ebola-saving-lives-natural-allopathic-medicine
28 November 2014 at 11:10 pm
Are you aware of the success of Drs. Robert Rowen, of Santa Rosa California and Howard Robins, of New York City, who have been teaching ozone therapy (direct Intravenous infusion of ozone gas) in Sierra Leone and have just announced the successful cure of a case of ebola in Sierra Leone using this therapy and other integrative methods. You can read about it here:
http://www.docrowen.com/ebola-cure-press-release.html
29 November 2014 at 11:33 pm
Well written article. Very informative. Sadly, Ebola is the new AIDS. It is an opportunity to incite fear and raise funds for organizations pretending to care about humanity.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences