Content Sections
This is a big subject, with big numbers and it’s about big waistlines – in a country that has espoused health equality for all since the inception of the National Health Service (NHS) in 1948.
Diabetes UK states that, “Blood glucose management in the UK is amongst the worst in Europe and around two thirds of all people with diabetes in England are not achieving the treatment targets recommended by National Institute for Health and Care Excellence (NICE).”
We say most of the money being spent on the ‘diabesity’ crisis is money misspent that’s not delivering the benefits that the public deserves given the current state of the science. This is the theme we tackle in our position paper, 'A Blueprint for Health System Sustainability in the UK' that we’ll be releasing for consultation next week. To understand why this is such an important issue, we’ve pulled together some of the numbers and graphics that show the scale of the problem.
If you’re moved by the issues, we would dearly like you to respond to our consultation, details about which you’ll find at the end this article.
The big number
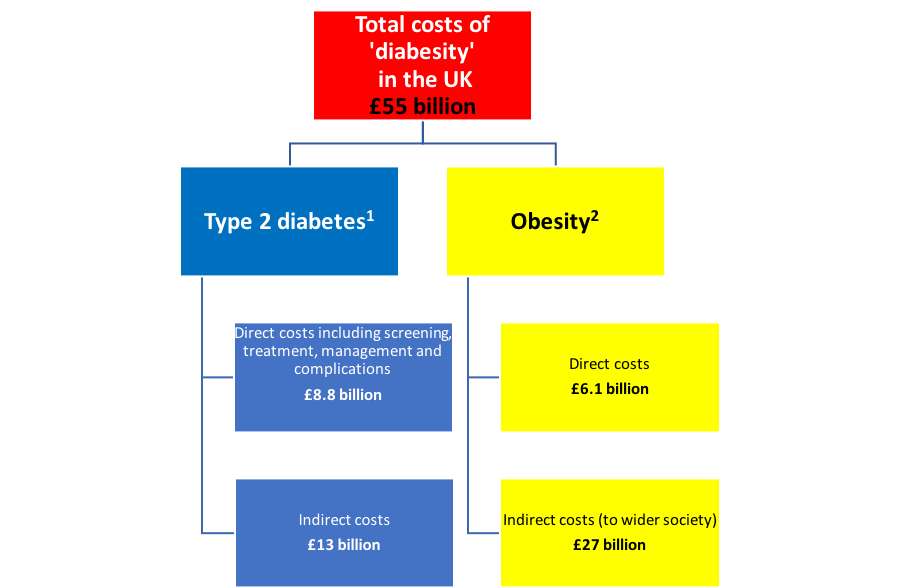
The big number when it comes to the estimated direct and indirect costs of just these two avoidable chronic diseases is as follows: it’s a cool £55 billion per annum (that’s €63 billion or US$77 billion). That works out at about £151 million per day, every day of the year.
Yes — and it’s avoidable.
Data sources:
1 Hex N, Bartlett C, Wright D, Taylor M, Varley D. Estimating the current and future costs of Type 1 and Type 2 diabetes in the UK, including direct health costs and indirect societal and productivity costs. Diabet. Med. 2012; 29: 855–862.
2 Public Health England. Guidance: Health matters: obesity and the food environment. 31 March 2017.
The scale of the UK’s obesity problem: Public Health England (PHE) infographics
The following images are sourced from Public Health England.
As a fraction of total NHS expenditure
- Net government expenditure on NHS was £121 billion in 2010/11
- The costs of diabetes represent approximately 10% of this budget
Source: Harker R. NHS funding and expenditure. House of Common Library, Standard Note: SN/SG/724. 3 April 2012. http://www.nhshistory.net/parlymoney.pdf
The cost of diet-related ill-health
- In 2006–07, poor diet-related ill health cost the NHS in the UK £5.8 billion.
- The cost of physical inactivity was £0.9 billion
Source: Scarborough P, Bhatnagar P, Wickramasinghe KK, Allender S, Foster C, Rayner M. The economic burden of ill health due to diet, physical inactivity, smoking, alcohol and obesity in the UK: an update to 2006-07 NHS costs. J Public Health (Oxf). 2011 Dec;33(4):527-35.
- Food related ill health is responsible for about 10% of morbidity and mortality in the UK and costs the NHS about £6 billion annually.
Source: Rayner M, Scarborough P. The burden of food related ill health in the UK. J Epidemiol Community Health. 2005 Dec;59(12):1054-7.
Hunting for solutions
Diabetes UK states that, “The best way to reduce the cost of diabetes is to prevent Type 2 diabetes in the first place.”
So far, the solutions being offered by government are piecemeal. They include efforts to improve better self-care, such as via the NHS’ One You project, and improving and reducing ‘out of home’ eating from fast food outlets, via the PHE toolkit, ‘Strategies for encouraging healthier “out of home” food provision.’
It’s just not enough.
The two policy goals of the Marmot Review from 2010 hit the nail on the head. They were: 1) to create an enabling society that maximises individual and community potential, and; 2) to ensure social justice, health and sustainability are at the heart of all policies.
Next week, we’ll be releasing our position paper, ‘Blueprint for health system sustainability in the UK’ for consultation.
At the heart of the position paper is a community based approach that resonates fully with Professor Michael Marmot’s policy goals. The position paper presents a disruptive, community-based approach that brings the locus of control for effective self-care and practitioner guided self-care back to the individual. It’s about focusing much more on upstream healthcare. None of this can happen if we don’t see a sea change in the way we go about healthcare – including altering public and medical establishment’s perception of the upstream causes of and triggers for the ‘diabesity’ epidemic.
Join our consultation
We’re initially looking for input from any organisation, practitioner or individual with an interest in the future of our healthcare – and particularly our ability to manage our own health – in the UK.
Nearly all the principles we’re working with are adaptable to other regions of the world – but initially we’re focusing on the UK. There are many reasons for this including because the UK is our geographic base, because Brexit, which presents both challenges and opportunities is imminent, because the diabesity crisis in the UK is so severe – and because of the presence of the NHS.
Please email our team at [email protected] and include ‘SHS consultation’ in the subject line. Please let us have your details, including your name, organisation, affiliation or your registration body if you’re a registered practitioner. We’ll make sure you receive by email week commencing 9 April the draft position paper, along with a short guideline document.
In early June we’ll be presenting the final form of the document and we’re looking to have as broad a support as possible so we can work to start implementing the ground-breaking recommendations.
Please share this widely with those who’re interested.













Comments
your voice counts
05 April 2018 at 12:39 am
I have sent an email to Jeremy Hunt, the Secretary of State for Health & Welfare, with an attachment that explains why we have the current problem with both obesity and type 2 diabetes. I tried to keep it brief. Would you like a copy to add to your research?
If you email me I can send a copy to you. It's only three pages.
Nick
05 April 2018 at 3:12 pm
Hello Nick
Thank you, that would be great. We will email you separately.
Warm Regards
Melissa
05 April 2018 at 10:03 am
Dr Jason Fung in Canada is curing diabetes and obesity with various forms of fasting.
05 April 2018 at 3:22 pm
That's great Carol, thank you for sharing Dr Fung's work with us.
Warm Regards
Melissa
05 April 2018 at 10:10 am
As a health and fitness professional I am committed to being part of the solution and will continue to support any initiative in this area.
Thank you for all your important work in this area...the nation's health depends upon it !!!!
05 April 2018 at 3:11 pm
Thank you Don, have you registered to be a part of our consultation. We'd love to hear your views.
Warm Regards
Melissa
05 April 2018 at 11:41 am
I am a neuro-developmental therapist and have worked for 25 years with children with a variety of specific learning difficulty. I use Applied Kinesiology as my diagnostic tool and I find that the three major deficiencies are iodine, zinc and magnesium. Many of the children I see are overweight. The link is that zinc is required for insulin production. Magnesium and zinc are required to activate vitamin B6 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4735993/ this paper demonstrates the importance of B6 on insulin.
Iodine is necessary to activate vitamin B2 through its role in thyroxin production. And active vitamin B2 is essential to activate the vegetable forms of vitamin B6. Without activation the vitamins cannot work. Thyroxin, magnesium and zinc are all part of the energy cycle so these children have less energy, expend less energy and don't feel well and will be more prone to comfort eating. We need to look at the mineral levels of our children and adults. It is known that the UK is iodine deficient in may areas. The research done in 2011 https//www.ncbi.nlm.nih.gov/pubmed/21640375 shows that many teenage girls are deficient and that as the future mothers their babies will be too and there is evidence to suggest that fat babies become fat adults.
05 April 2018 at 3:11 pm
Thank you for taking the time to comment Sue, it's always appreciated.
Warm Regards
Melissa
06 April 2018 at 7:37 am
You need to take low quality produce and sugar out of Big food, at manufacturing level;
boost organic farming so that local organic growers produce becomes the norm not the exception, this means over time increase demand and availability so that also price lowers.
Make sure Organic certification means certified non GMO organic so that produce is not passed for organic when it's not and sneaky caveats are introduced to add chemicals but still calling it organic.
educate people about their biochemistry so that there is a bottom up change in personal accountability to understand and implement long term change habits for ones lifestyle ( Soil Association initiatives being one really good way to bring education in schools, amd for parents amongst all the others)
AND a top down change that promotes actual health not sugar, unnecessary goods where there is no disposable income available due to poverty. This is fundamental as a governevent responsibility towards long terms health which is and has been a statutory requirement in the Act since the start.
In a balanced concurrent approach health can still be accessible on the basis we used to have it where personal accountability can mean less disease.
Re-education in nutrition of the health profession away from synthetic pharmacology being the only go to for treating disease.
Access to nutrition and health education and information that is science based not biased by business interests.
If eventually there is a shift towards considering genetic testing for a personalised and maybe ? more accurate approach towards nutrition, appropriate regulation must be put in place to safeguard people's personal data so this is not used against them by the medical, insurance or other systems.
Because lifestyle doesn't only involve sugar and food, also address the other areas that have over time destabilised people's biology ( high cortisol, low dopamine etc..), in other words simplify life and re prioritise necessities.
Prioritise employment and fair work rapport, long term stability, structure and access to give people the stability they need to then consider health.
Currently and I don't want to sound one sided saying this there is a policy forum that the Labour Party has set up for people to contribute their ideas to policy making.
Because we are all part of this society and because we all need to take responsibility for how it turns out and may change, I personally felt that the policy forum is a good idea.
No point complaining about it all but then not being prepared to pull head out of sand and make a contribution towards its change.
06 April 2018 at 10:27 am
Hi Melissa
We've received funding from the Diabetes Innovation & Improvement Fund to run a programme for type 2 diabetics. We'll be getting them to eat better (less processed - especially carbs), get more active and are linking up with a clinical psychologist to have input on behavioural change and stress management. It's a weekly 3 hour session for 6 weeks with a follow up at 12 & 24 weeks. We're measuring HBA1c and CRP to monitor any changes.
I've emailed you for a copy of the consultation.
Kind Regards
Eoghan
10 April 2018 at 11:23 am
Hi Eoghan
This is great news, very encouraging. Please do keep us posted on developments and results. We'd definitely consider publishing an article or case study if you're up for that once the trial is over?
Best wishes
Meleni
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences